Psoriasis
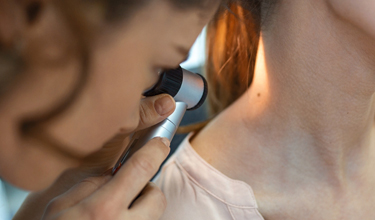
Psoriasis is a chronic autoimmune condition that primarily affects the skin. It is characterized by the rapid growth of skin cells, leading to the formation of thick, red, scaly patches that can be itchy or painful. These patches, known as plaques, can appear anywhere on the body but are most commonly found on the elbows, knees, scalp, and lower back. It affects 3% of the US adult population or more than 7.5 million adults.
Psoriasis typically follows a pattern of flaring for a few weeks or months, then subsiding for a time or going into remission. Triggers for psoriasis flares can vary and may include stress, certain medications, dry weather, or skin injuries.
The severity of psoriasis varies among individuals and can have a significant impact on a person’s quality of life, including emotional and physical aspects. It is also associated with other serious health conditions, such as psoriatic arthritis, cardiovascular disease, and diabetes.
However, not every individual with psoriasis will experience these additional health issues. Both psoriasis and its associated comorbidities can exert a significant detrimental effect on an individual’s quality of life.
Plaque Psoriasis is the most common form, characterized by raised, red patches covered with a silvery white buildup of dead skin cells. It is typically found on the knees, elbows, lower back and scalp. The plaques feel tight, burn, sting or itch, crust, may crack and bleed, and cause pain. These plaques can affect the scalp, eyebrows, the skin between the nose and lips and the forehead. It can also cause pitting of the nails.
What causes psoriasis?
The exact cause of psoriasis is not fully understood, but it is believed to be related to an immune system malfunction. In people with psoriasis, the immune system mistakenly attacks healthy skin cells, speeding up the skin cell production process. Instead of taking weeks for skin cells to develop and shed, this process happens in just a few days. The excess skin cells then build up on the skin’s surface, forming the characteristic plaques.
In addition to immune system malfunction, genetics and environmental factors play a role. Psoriasis runs in families. Environmental factors can trigger psoriasis in individuals who are genetically predisposed to the disease. Common triggers include cuts, bug bites and severe sunburns. Stress can exacerbate psoriasis. Some medications can trigger psoriasis. Cold and dry weather can lead to flareups. Smoking and heavy alcohol consumption can increase severity.
What are the treatment options?
The treatment options for psoriasis are diverse and are often selected based on the severity of the condition, the size of the areas involved, the type of psoriasis, and the patient’s response to initial treatments.
Topical Treatments
These are applied directly to the skin and are usually the first line of defense, particularly for mild to moderate psoriasis.
- Corticosteroids: These are the most frequently prescribed medications for treating mild to moderate psoriasis and work by reducing inflammation and relieving itching.
- Vitamin D analogues: These synthetic forms of vitamin D slow down the growth of skin cells.
- Retinoids: Topical retinoids are vitamin A derivatives that can help improve psoriatic skin changes.
- Calcineurin inhibitors: Generally used for the treatment of atopic dermatitis, they can be effective for psoriasis in sensitive areas such as around the eyes, where steroids are not recommended.
- Salicylic acid: This can help remove scales and is often combined with other medications.
Phototherapy (Light Therapy)
This involves exposing the skin to ultraviolet light under medical supervision.
- UVB phototherapy: Treatment with either broadband UVB or narrowband UVB light can help to slow the abnormal growth of skin cells.
- Psoralen plus ultraviolet A (PUVA): This treatment involves taking a light-sensitizing medication (psoralen) before exposure to UVA light.
- Excimer laser: A form of light therapy that targets only the affected skin without harming healthy skin.
Systemic Medications
These are prescription medications that are taken orally or by injection and are used for more severe psoriasis or when other treatments are ineffective.
- Methotrexate: Slows cell turnover by suppressing the immune system.
- Cyclosporine: Suppresses the immune system and is similar to methotrexate in effectiveness.
- Biologics: These drugs, which are typically administered by injection, alter the immune system and have been very effective in treating psoriasis. They target specific parts of the immune system that drive inflammation in psoriasis.
- Oral retinoids: These are used for severe psoriasis and have significant effects on the skin cell production cycle.
- Apremilast (Otezlaâ): This oral medication reduces inflammation.
Lifestyle Changes and Complementary Therapies
These can be beneficial alongside medical treatments.
- Regular moisturizing: Keeping skin moist with heavy creams or ointments can help control flare-ups.
- Dietary modifications: Some patients report improvement with a diet low in inflammatory foods or gluten.
- Stress management techniques: Stress reduction can help prevent or reduce the frequency of flare-ups.
- Avoidance of triggers: Identifying and avoiding triggers is an important part of managing psoriasis.
Medical dermatologist Dr. Sheila Farhang will work closely with you to identify triggers and determine the most appropriate treatment or combination of treatments to help you live a better life with psoriasis. Contact her at Avant Dermatology & Aesthetics in the Tucson (Orzo Valley) to schedule a consultation today.





 / 291 Reviews
/ 291 Reviews
socialize with avant
#naturalskin